- Blog
- Drop shadow font in after effects
- Fatehollow ataraxia eclipse scenario life of sakura
- Diablo 1 download free full version
- Bejeweled 2 play free online with music
- Microsoft outlook 2014 change email signature
- Ds 160 form angola
- Cellar spider daddy long legs bodies
- Sample budget for a person on ssi
- Omnisphere challenge code keygen mac
- Houston county 411 gazette
- Ged maths practice questions
- Immortals 2011 full movie online free
- Softonic minecraft pocket edition pc
- Microsoft access sample database aspnet
- Montreal cognitive assessment moca test scoring verywell
- Ms subbulakshmi tamil suprabhatam free download
- Hard and soft signs trauma
- Ptcl bandwidth speed test
- Embed video autoplay gmail email
- Pcclone ex lite driver download win 10
- Best live wallpaper software windows 10
- Content control microsoft word template
- Gun crosshair transparent background
- Dsm 5 main criteria in diagnosing ptsd
- Afterglow ps3 pc controller
- Pixelmon kanto map 1-12-2
- Imvu redeem codes 2020 free
- Fortnite save the world free redeem codes
- Quicktime player for pc free download
- Hyde bar flavors
- Guitar hero live controller wii u
- Seven habits of highly effective people paradigm
- Farming simulator 19 cop car
- Free download ccleaner for windows 10
- Free christmas propresenter backgrounds
- Custom soul calibur 5 characters funny
- 1st grade sight word bingo
- Annual expense report template
- Monica garcia susan rubio
- Softonic minecraft pocket edition 2021
- Macaroni and cheese instant pot
- Pdf xchange editor pro keygen
- Pi filter calculation design
- Cursive font generator tattoo
- Vrchat thicc avatar worlds
- Rgh xbox emulation on 360
- Ptsd dsm 5 criteria a h listed
- Watch assassination classroom episode 1 gogoanime
- Top pc monitoring software for parents-

The classical six P's of ischaemia: pain, pulselessness, pallor, paraesthesias, poikilothermia and paralysis if present go to reinforce the diagnosis but unfortunately may not be present in all cases especially in injuries to the axillary and brachial arteries where the radial pulse may be palpable 7. Strict clinical criteria have to be adhered to in order to achieve this. Recognition of arterial injuries is of paramount importance if limbs and lives are to be preserved. Injuries to peripheral vessels are also usually associated with injuries to accompanying nerve trunks and may also be extensive to involve muscles, tendons and even bones and joints which go to increase the morbidity associated with these injuries. These injuries may be neglected or missed with the result of considerable morbidity with loss of limb and mortality. 5, 6 The real incidence in Ghana and probably the rest of the West African region may not be known due to low reporting. 3, 4 Vascular trauma has also gained prominence in recent times due to interventional procedures performed on arteries and veins and such iatrogenic injuries are the commonest causes of vascular injuries in certain parts of the western world. These injuries are, however, common in certain parts of South Africa 1, 2 and the United States of America. 2006 60(2):432–42.Traumatic injuries to major peripheral vessels in civilian life are quite uncommon worldwide. Extremity vascular injuries on the battlefield: tips for surgeons deploying to war. Starnes BW, Beekley AC, Sebesta JA, Andersen CA, Rush RM Jr. 2010 16(6):602–8.Īmerican College of Surgeons COT: ASSET-advanced surgical skills for exposure in trauma. Management of peripheral arterial injury. Use of substitute conduits in traumatic vascular injury. Lau JM, Mattox KL, Beall AC Jr, DeBakey ME. Management of lower extremity arterial trauma. Martin LC, McKenney MG, Sosa JL, Ginzburg E, Puente I, Sleeman D, et al. Five-year experience with PTFE grafts in vascular wounds. Western Trauma Association critical decisions in trauma: evaluation and management of peripheral vascular injury, part II. 2009 46(10):779–839.įeliciano DV, Moore EE, West MA, Moore FA, Davis JW, Cocanour CS, et al. discussion 519–22ĭente CJ, Wyrzykowski AD, Feliciano DV. Non-invasive vascular tests reliably exclude occult arterial trauma in injured extremities. Evaluation and management of penetrating lower extremity arterial trauma: an Eastern Association for the Surgery of Trauma practice management guideline. 2011 70:1551–6.įox N, Rajani RR, Bokhari F, Chiu WC, Kerwin A, Eastern Association for the Surgery of Trauma, et al. Western Trauma Association/critical decisions in trauma.
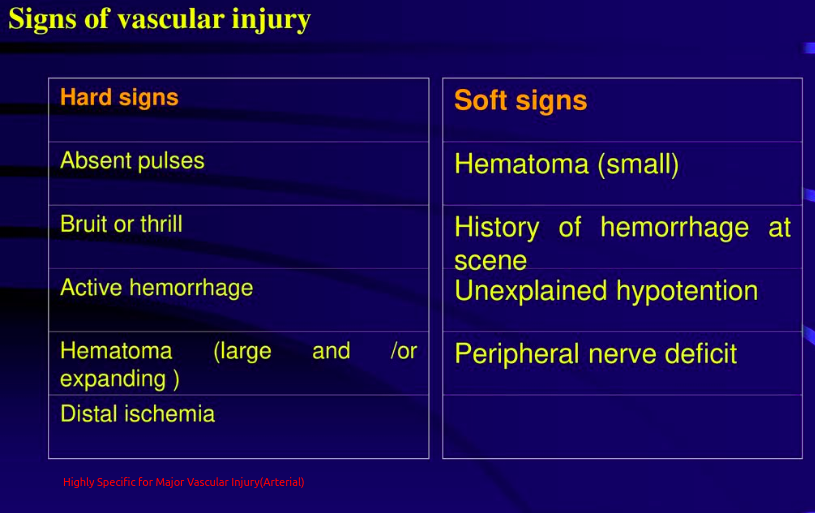
Evaluation and management of peripheral vascular injury: part 1. Keywordsįeliciano DV, Moore FA, Moore EE, West MA, Davis JW, Cocanour CS, et al. A number of damage control options exist in the setting of complex injury or physiologically compromised patients, which include temporary shunting or ligation. In regions of difficult anatomy, endovascular and open techniques can be combined in a hybrid approach to minimize morbidity. Recently, endovascular options for vascular control and definitive management of vascular injuries have emerged. The operative principle of proximal and distal control is critical and has traditionally been achieved via classical open operative exposures. Hard signs in general mandate exploration, whereas soft signs permit more further workup. Life-threatening bleeding may come from a vascular injury or from elsewhere. Patient assessment begins with identification of all life-threatening injuries followed by the identification of hard and soft signs of vascular injury. Vascular injury management is a fundamental skill for trauma surgeons.
